-
三尖瓣反流表现为三尖瓣或三尖瓣环结构上的异常,导致一部分血流从右心室反流回右心房,通常由原发性或肺动脉高压、房颤、左心瓣膜疾病导致的继发性功能障碍所致[1]。手术是目前治疗三尖瓣重度反流的最佳选择[2]。胃肠功能障碍是心胸外科手术患者术后常见并发症,且早期胃肠功能障碍患者更容易出现术后机械通气时间延长、重症监护室(ICU)住院时间延长等问题[3]。胃肠动力药是促进患者术后胃肠功能恢复的常见用药,能有效缓解患者术后消化功能紊乱症状。笔者选择2011年1月至2021年12月海军军医大学第一附属医院心血管外科收治的184例三尖瓣重度反流患者,观察并分析术后3 d内预防性使用胃肠动力药在体外循环下三尖瓣置换术患者的临床治疗效果,现报告如下。
-
本研究为回顾性分析,纳入对象为2011年1月至2021年12月于我院收治的重度三尖瓣反流患者。纳入标准:①患者临床诊断为重度三尖瓣反流;②患者接受体外循环下三尖瓣置换手术。排除标准:①手术后3 d内死亡患者;②手术后3 d内出现消化道症状的患者。共收集符合纳入标准的重度三尖瓣反流患者184人,其中,男性患者76例(40.98%),中位年龄54.0[47.0,66.0]岁,女性患者108例(59.02%),中位年龄60.0[52.0,66.0]岁。
-
患者入院后,行术前常规检查。对符合手术指征且有手术意愿的患者采用胸部正中切口或右胸外侧切口进行手术。手术过程中对患者建立体外循环,行生物瓣或机械瓣置换术。术后于我院心外科ICU进行进一步治疗。
-
收集患者的人口统计学资料,包括年龄、性别、疾病史等,术后3 d内胃肠动力药服用情况,术后首次排便时间,手术3 d后胃肠道相关症状,手术3 d后急性肾衰竭、肺部感染、脑卒中等并发症发生情况。此外,收集并记录患者ICU住院时间、机械通气时间、胃管置入时间。
-
术后3 d内服用胃肠动力药定义为预防组,术后3 d内未服用胃肠动力药定义为对照组。排便延迟判定:术后3 d内(包括第3天)排便为正常排便,术后3 d以上排便为排便延迟。
-
采用SPSS 21.0 统计学软件进行数据统计分析。符合正态分布的计量资料采用t检验进行统计,以(
$\bar x $ ±s)表示;不符合正态分布的计量资料采用非参数分析进行统计,以中位数(四分位数间距)[M(QL ~ QU)]表示。计数资料采用卡方(χ2)检验进行统计,以例数(百分比)[n (%)]表示。P<0.05表示差异具有统计学意义。 -
在纳入研究的184例重度三尖瓣反流患者中,有101例患者(54.89%)术后3 d服用胃肠动力药,其中,72例患者(39.13%)术后服用莫沙必利,36例患者(19.57%)术后服用多潘立酮,7例患者(3.80%)同时服用莫沙必利和多潘立酮;83例患者(45.11%)术后3 d内未服用胃肠动力药。两组患者在年龄、性别、BMI、疾病史、手术史均无统计学差异(P>0.05),见表1。
项目 预防组 对照组 χ2(Z)值 P值 年龄 (岁) 56.0 [51.0,67.0] 59.0[49.0,65.0] −0.039 0.970 男性[n (%)] 40 (39.6) 36 (43.4) 0.267 0.653 BMI (kg/m2) 22.5 [20.4,24.0] 21.7 [19.0,23.9] −1.744 0.081 糖尿病[n (%)] 8 (7.9) 6 (7.2) 0.031 1.000 高血压[n (%)] 12 (11.9) 8 (9.6) 0.237 0.645 肝硬化[n (%)] 3 (3.0) 4 (4.8) 0.426 0.703 肾功能不全[n (%)] 3 (3.0) 1 (1.2) 0.668 0.628 脑卒中史[n (%)] 5 (5.0) 8 (9.6) 1.525 0.256 心脏手术史[n (%)] 79 (78.2) 57 (68.7) 2.152 0.177 -
预防组患者术后平均首次排便时间为3.32 d,低于对照组患者术后平均首次排便时间4.67 d。预防组患者中排便延迟的发生率为40.1%,显著低于对照组患者排便延迟发生率65.1%,差异均具有统计学意义(P<0.05),见表2。
项目 预防组 对照组 χ2(Z)值 P值 排便时间 (t/d) 3.0[2.0,4.0]*** 4.0[3.0,5.0] −3.634 <0.001 排便延迟[n (%)] 41 (40.6)** 54 (65.1) 10.920 0.001 **P<0.01,***P<0.001,与对照组比较。 -
预防组患者腹胀症状发生率明显低于对照组患者,差异具有统计学意义(P<0.05),其他胃肠功能障碍未见统计学差异(P>0.05),见表3。
项目 预防组[n (%)] 对照组[n (%)] χ2(Z)值 P值 恶心 11 (10.9) 10 (12.0) 0.060 0.820 呕吐 9 (17.8) 5 (6.0) 0.540 0.581 腹胀 2 (2.0)* 8 (9.6) 5.199 0.045 腹泻 3 (3.0) 6 (7.2) 1.776 0.303 消化道出血 4 (4.0) 3 (3.6) 0.015 1.000 *P<0.05,与对照组比较。 -
预防组患者肺部感染发生率显著低于对照组患者(P<0.05),其余术后并发症未见统计学差异(P>0.05)。此外,预防组患者ICU时长、气管插管时长、胃管置入时长均短于对照组患者,差异具有统计学意义(P<0.05),见表4。
项目 预防组 对照组 χ2(Z)值 P值 死亡[n (%)] 6 (5.9) 9 (10.8) 1.463 0.283 心功能不全[n (%)] 4 (4.0) 3 (3.6) 0.015 1.000 肾衰[n (%)] 5 (5.0) 10 (12.0) 0.080 0.105 肺部感染[n (%)] 5 (5.0)* 12 (14.5) 4.911 0.039 癫痫/脑卒中[n (%)] 3 (3.0) 4 (4.8) 0.426 0.703 ICU时长 (t/h) 100.0[25.5,85.0]* 176.5[43.0,119.0] −2.190 0.028 气管插管时长 (t/h) 41.0[7.0,21.5]** 126.0[15.0,44.0] −3.127 0.002 胃管置入时长(t/h) 67.0[10.5,26.0]** 143.0[17.0,82.0] −3.191 0.001 *P<0.05,**P<0.01,与对照组比较。 -
重度三尖瓣反流患者常伴有严重的右心衰竭,可能引起患者内脏静脉压长期升高,从而导致患者肠细胞长期缺血和肠屏障功能的破坏[4]。此外,肠黏膜血流在正常生理条件下为黏膜细胞提供足够的氧气和营养,以维持正常的消化功能,而在体外循环的条件下,例如手术后,可能会出现肠黏膜缺血和再灌注损伤,引起患者肠通透性增加和屏障功能受损,导致胃肠蠕动功能降低[5-7]。在本研究中,肠功能紊乱可能是接受体外循环下三尖瓣置换手术患者排便延迟的重要原因。术后胃肠功能障碍增加了住院时间、护理成本和术后发病率。因此,对于体外循环下三尖瓣置换术患者术后应进行早期胃肠功能干预。
本研究排除了手术后3 d内发生消化道症状的患者。这些患者在发生不良反应后通常采用多种手段辅助治疗,这可能会影响对胃肠动力药预防效果的判断,故不纳入本研究。胃肠促动药能够加强胃肠蠕动,促进胃排空,协调胃肠运动,主要用于治疗胃肠道疾病,如功能性消化不良,胃食管反流病,糖尿病性胃轻瘫和术后肠梗阻[8]。本研究中选用莫沙必利和或多潘立酮作为胃肠动力药给药方案,其中莫沙必利给药剂量为5 mg,每日3次;多潘立酮给药剂量为10 mg,每日3次。莫沙必利是一种选择性5-HT4受体激动剂,通过兴奋胃肠道5-HT4受体,从而增加乙酰胆碱的释放,促进患者胃肠道蠕动和排空[9]。多潘立酮是一种多巴胺受体拮抗剂,由于其对胃和小肠的化学感受器触发区和运动功能的影响,常被充当为止吐剂和胃肠促动力剂[10]。同莫沙必利或多潘立酮单独使用相比,二者联合应用有助于患者术后胃肠功能的早期恢复,但可能会增加患者腹泻风险[11]。本研究表明,胃肠动力药在术后3 d内预防性使用,能有效促进三尖瓣置换术后患者的排便,降低排便延迟的发生率。合理的术前生活方式和饮食措施、术后胸段硬膜外镇痛、水电解质平衡、口香糖咀嚼、预防性使用泻药也可作为预防术后排便延迟的有效措施[12, 13]。对于已经出现排便延迟的患者,渗透性或黏液性泻药、促动力药物和维持水电解质平衡等干预措施对缓解症状具有重要意义[14]。
在危重患者的管理中,胃肠动力障碍会继发许多并发症,如反流或误吸导致肺功能降低和呼吸机相关性肺炎、营养不良、败血症等[15]。本研究发现,预防性服用胃肠动力药能有效降低三尖瓣置换术患者术后肺部感染的发生率,并降低术后ICU、机械通气和胃管置入的时间。目前,有研究表明莫沙必利对胃造瘘术患者预防肺炎的有益作用[16]。此外,定期给予多潘立酮可降低急性缺血性卒中患者吸入性肺炎的发生率,缩短住院时间,改善短期临床结局[17]。因此,莫沙必利和多潘立酮等胃肠动力药的促动力作用在三尖瓣术后患者中预防吸入性肺炎方面可能扮演重要作用,值得临床推广和使用。
Observation of the prophylactic use of prokinetic agents in patients after tricuspid valve replacement under cardiopulmonary bypass
doi: 10.12206/j.issn.2097-2024.202210060
- Received Date: 2022-10-31
- Rev Recd Date: 2023-04-09
- Available Online: 2024-03-20
- Publish Date: 2024-03-25
-
Key words:
- prokinetic agents /
- tricuspid valve replacement /
- clinical effect /
- retrospective study
Abstract:
| Citation: | CHEN Qian, XU Xiangyang, LU Fanglin, HAN Lin, LI Bailing, XU Zhiyun. Observation of the prophylactic use of prokinetic agents in patients after tricuspid valve replacement under cardiopulmonary bypass[J]. Journal of Pharmaceutical Practice and Service, 2024, 42(3): 131-134. doi: 10.12206/j.issn.2097-2024.202210060 |








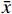
 DownLoad:
DownLoad: